Liver metastases
Introduction
The liver is one of the organs most frequently affected by metastases from malignant tumors in other parts of the body
Stereotactic body radiotherapy (SBRT) is an innovative and painless technique. It is non-invasive and done outpatient, allowing for the rapid return of the patient to a normal life
The liver is one of the organs most frequently affected by metastases from malignant tumors in other parts of the body (primarily the breast, lung and colon).
The liver is the only organ affected by metastatic disease in the case of colorectal cancer in a large number of patients. In these cases aggressive local treatments may be indicated in order to remove these lesions.
Approximately 20% of patients diagnosed with colorectal cancer show signs of liver metastases present at the time of diagnosis. Metastases usually occur in the majority of the cases, up to 50%, after the completion of the treatments on the primary tumor. These percentages are directly related to tumor characteristics and its stage at the time of diagnosis. It can be said that there is a lower likelihood of developing liver metastases in early detection of the primary tumor.
Symptoms
Metastatic lesions in the liver appear are asymptomatic. They are commonly detected in periodic checkups or in a spread study of a primary tumor.
At other times Signs and symptoms such as pain in the right side of the abdomen or yellowing of the skin due to obstruction of the biliary tract appear at other times.
Diagnosis
Diagnosis is usually obtained from imaging studies and blood tests (tumor markers such as CEA and CA 19-9). A strict follow-up protocol must be done for this reason after treatment of a primary tumor for the early detection of possible liver involvement.
Additional specific imaging tests for the diagnosis of metastatic lesions in the liver are:
- Abdominal ultrasound is done by a medical specialist who carries out an examination of the entire abdomen using an ultrasound probe to obtain images of the liver and adjacent organs. It is a safe, painless, effective and quick test.
- Computed tomography (CT): Images are obtained after the administration of a radiopaque contrast for identifying the presence of liver metastases.
- Positron emission tomography (PET with FDG): the degree of metabolic activity of metastatic lesions can be seen with this test.
- Magnetic resonance imaging (MRI) is the imaging technique that has demonstrated greater accuracy in the detection of liver metastases and better able to differentiate them from other nonspecific lesions. It is performed in selected cases after the CT or as an alternative for a more precise definition of the number, size, location and nature of the lesions which can affect treatment decisions.
Surgery
The surgical indications for removal of hepatic metastases depend largely on the number, location and spread of the metastases as well as the absence of disease elsewhere in the body.
Surgery of liver metastases can be performed with ultrasound guidance. The surgeon is able to accurately identify the location of the lesion facilitating their complete removal of while preserving the maximum amount of healthy liver tissue.
Radiotherapy
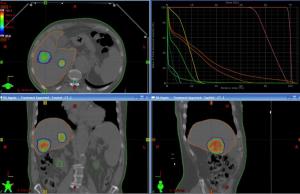
A selective treatment of liver lesions can be done in chosen patients by administering stereotactic body radiotherapy (SBRT). This technique directs high doses of radiation to the lesions in only a few treatment sessions.
iTAcC has the most advanced technology and precise treatments for this type of radiotherapy. With the TrueBeam STX © system we can carry out stereotactic body radiotherapy (SBRT) and Image-guided radiotherapy (IGRT) techniques, as well as detect respiratory movements of the patient. The prescribed treatment is administered with sub-millimeter precision while preserving the highest possible percentage of healthy liver tissue.
Chemotherapy
Neoadjuvant chemotherapy is administered prior to the removal of metastases in order to reduce their size and number.
Adjuvant chemotherapy is administered after the surgery in order to reduce the risk of disease recurrence.
Chemotherapy is administered in cases where it is not possible to carry out radical surgery in order to increase the chances of bringing the disease under control. This treatment is completed in many cases using biologic drugs which permits an increased tumor response.
Intra-arterial therapy (chemoembolization)
This technique is primarily used in patients who are unable to undergo other treatments. The blood vessels supplying the tumor are identified and chemotherapeutic agent is injected causing the blood flow to become obstructed thereby increasing the antitumor effect.
The embolization procedure may represent a particularly important therapeutic option in the presence of certain types of metastatic tumors (neuroendocrine).
Radiofrequency
This technique involves the ablation of lesions through the application of heat. This is achieved by raising the temperature generated by the passage of current. It can be performed by laparoscopy, open surgery or percutaneously by injecting vectors guided by ultrasound, through the abdominal wall. The procedure is performed under anesthetic sedation in the operating room with ultrasound control.
Research
At iTAcC we foster a strong interest in research within the context of clinical protocols allowing for the development of new therapies and improve existing ones. Our goal is to increase the patient’s survival rate and improve the quality of life for those patients diagnosed with liver cancer.
Follow up
The multidisciplinary team establishes a customized control plan after treatment. It is done according to the needs of each patient and the biology of the disease in order to rule out or for early detection of any recurrence. The follow up is done based on a comprehensive control of the tumor by imaging tests and an analysis of liver function.
Follow up is done as in the case of all oncological activity at iTAcC, in a personalized manner with cooperation of doctors who have been involved in the diagnosis and treatment of each case. iTAcC is an open institution and works closely them.


