Lung cancer
Introduction
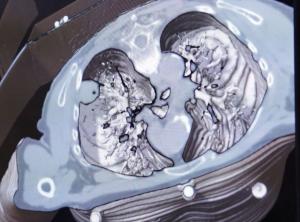
Lung cancer is the leading cause of death in industrialized countries. Smoking is the leading cause of lung cancer in both active smokers (representing 85% of patients) and among those who are exposed to passive smoke. The risk of disease increases with the number of years that the individual has smoked. Quitting smoking even after many years, reduces the risk of lung cancer significantly.
Tobacco smoke contains carcinogens that damage the cells lining the alveoli. It is repaired initially but over time the injury is irreparable and a tumor may result. The causes of the disease are not entirely clear in the case of non-smokers or people with little exposure to tobacco smoke. Alterations in genes involved in the development of lung tumors have been identified.
Virtual navigation in the chest in order to see a lung tumor
The main types of lung cancer are:
Non-small-cell lung carcinoma.
- Adenocarcinoma (not related to the consumption of tobacco).
- Squamous cell or epidermoid carcinoma.
- Large cell carcinoma.
Small cell carcinoma
Less common and more associated with smoking.
ABC Newspaper: The importance of reducing time in lung cancer (article)
Risk factors
The main risk factors for lung cancer include:
- Active smoking is the most important
- Exposure to second hand tobacco smoke (passive smoking).
- Exposure, often for work related reasons, to substances such as radon, asbestos, arsenic, nickel, coal, chrome.

Prevention
Diagnosis
The diagnosis of lung cancer begins with a complete medical evaluation. It is reached after performing a biopsy and the samples are analyzed by a pathologist. Carrying out a comprehensive study to determine the real extent of the disease is very important as well. All this information together helps your doctor evaluate your situation. He or she will be able, along with other specialists, define the treatment of choice in your case.
ITAcC specialists are able to administer all the necessary tests for the purpose of defining what the best treatment is in each case. The tests involved in personalizing a treatment are:
Diagnostic imaging
A chest x-ray, CT, PET-CT, bone scan and MRI can be done to determine the nature of the lung lesion and the extent of disease.
Procedures for pathologic sampling
Diagnosis of lung cancer: tissue samples (biopsy) and the cytology are obtained by various tests and procedures which include:
Bronchoscopy
The bronchoscopy is a thin, flexible instrument that is inserted by the (respiratory specialist) pulmonologist under local anesthesia through the nose or mouth. It is used to look inside the lungs as well as extract a tissue sample in order to perform a histological and cytological study.
Transbronchial and transesophageal endoscopic ultrasound
This method consists in performing an aspiration endoscopically guided by ultrasound. This allows the specialist to take tissue samples from the lymph nodes through the airways or esophagus.
Needle aspiration and biopsy
Under local anesthesia a thin needle is inserted into the tumor in a lymph node or other tissue. This is done in order to take a sample of cells. This test is performed controlled by a CAT in order to ensure that the needle reaches the tumor.
Mediastinoscopy
This test is performed under general anesthesia. An instrument is inserted through a small incision into the base of the neck for a biopsy of the lymph nodes in the chest cavity. In this way it is possible to determine the stage of the tumor and whether surgery is needed. This test is being done less and less because it is being replaced by PET-CT, a non-invasive and highly diagnostic test.
Thoracentesis
If there is fluid in the thoracic cavity at the time of diagnosis then a sample can be collected by introducing a needle between two ribs to reach the pleural cavity. The liquid is used for the purpose of performing a cytological examination. This determines the presence of tumor cells in the pleural fluid. When there is a lot of liquid, this procedure may also be used to remove a quantity of liquid sufficient in order to improve the patient’s breathing.
Videothoracoscopy
A micro-camera is inserted under general anesthesia through a small incision in the chest to see the pleural surface. Tissue samples are then taken for a histological examination.
Lung function tests
A respiratory function test is used to determine lung capacity and functional reserve. These data allow specialists to determine whether the patient can tolerate surgery or extensive radiotherapy treatment.
Blood analysis
Treatment
At iTAcC pulmonologists, thoracic surgeons, oncologists, radiotherapists, pathologists, and other medical specialists combine their expertise in order to select the most appropriate treatment for each patient on an individual basis in the context of international scientifically approved protocols.
Various therapeutic options are evaluated according to the following factors: histological type of tumor, extent of the disease and the patient’s general health.
The different options individually, sequentially or complementary are:
Surgery
Surgery is the treatment of choice in many cases of non-small cell lung cancer. The different procedures are:
- Wedge resection: it is the removal of the tumor by extracting a small part of the lung which includes the tumor. It can be performed with minimally invasive surgical techniques (thoracoscopy).
- Segmental resection: it is a resection of a segment (part of a lobe) of the lung.
- Lobectomy: This involves the removal of an entire lobe of the lung. A lobectomy associated with lymphadenectomy (removal of lymph nodes) is the most common type of surgery for lung cancer.
- Bronchial resection with the placement of a bronchial prosthesis. This technique is used in with endobronchial tumors or those situated between two lung lobes. It permits the preservation of the lung lobes within oncological radicality.
- Pneumonectomy is the removal of the entire lung.
- Minimally invasive surgery: it can be used in select cases for thoracoscopic lung resection.
Thoracic surgeons who collaborate with iTAcC make up a highly specialized team in the treatment of lung cancer.
Radiotherapy
Radiotherapy treatment of lung cancer is done almost exclusively by external radiation energy source.
Specialists will design a customized treatment plan for the individual patient based on the type of tumor, its extent and the health condition of the patient. The most modern tools that technology has to offer such as the PET-CT are used in order to determine the true extent of the disease.
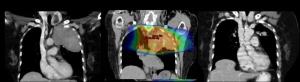
Treatments can be administered in combination with surgery (before or after) as well as simultaneously or sequentially with chemotherapy.
iTAcC has a team of highly experienced professionals in SBRT (stereotactic body radiotherapy). This technique concentrates a high dose of radiation with sub-millimeter accuracy causing tumor destruction. It is performed with the Truebeam STx (superior to other robotic systems) system and has proven very effective in killing small tumors or lung metastases with minimum tissue damage to surrounding healthy tissue. This therapy is used primarily for patients with small tumors who are not candidates for surgery because of the presence of other diseases in which it is contraindicated. It is also used as well as in cases of lung metastases.
Chemotherapy
There are multiple active drugs in lung cancer. They can be administered in combination with one another or by themselves in some cases.
Medical oncologists at iTAcC evaluate each case individually within the context of a multidisciplinary committee. The most appropriate treatment will be defined in each case based on the different biological and genetic characteristics of the tumor.
An “adjuvant” treatment is a possibility when chemotherapy is administered after radical surgery in order to reduce the risk of disease recurrence.
Chemotherapy “neoadjuvant” can be carried out before surgery in cases when the tumor is not operable from the start. This is due to the extension of the disease. It is administered along with radiotherapy with the aim being to shrink the tumor to make it operable. This allows for a more conservative surgery.

Chemotherapy is administered as a treatment complemented by radiotherapy in cases where the tumor is already involved with other organs such as bone, liver, etc. in order to slow the progression of the disease and improve the patient’s quality of life.
Biological therapies
Some lung tumors over-express certain biological characteristics in their cells. This opens up a field of possibilities in the treatment of this disease, one in which the specialists of our institution have vast experience.
Biological treatments used most often in lung cancer are those directed against the epidermal growth factor receptor (EGFR) and are administered orally (gefitinib, erlotinib).
Bevacizumab is another biological agent containing compounds derived from platinum. It is used in select cases in combination with chemotherapy. It is a monoclonal antibody directed against the vascular endothelial growth factor (VEGF).
At iTAcC we are able to perform an analysis of tumor DNA to determine its mutations (study of the EGFR gene mutation). This is used to check the patient’s sensitivity regarding this type of treatment.
Follow-up
iTAcC has the means to monitor and control the progress of patients who have had lung cancer in order to rule out the possibility of disease recurrence.
Follow up is done as in all oncological activity at iTAcC in a personalized manner with cooperation of doctors who have been involved in the diagnosis and treatment of each case. iTAcC is an open institution and works closely these specialists.
Patients may require therapist guided rehabilitation in the recovery of their respiratory function after surgery.


